what nutritional deficiency contributes to osteoporosis in older adult patients?
Levels necessary for os health
The threshold for the level of vitamin D to optimise a range of wellness outcomes remains controversial and randomised controlled trial bear witness to support aiming for high levels is very limited. For bone wellness and muscle function, the optimal level appears to be ≥50 or lx nmol/L, using the higher value if measured in summer to allow for seasonal decrease.1 A cut-off of 50 nmol/50 remains appropriate to define deficiency,1,2 with farther classification into astringent (<12.5 nmol/L), moderate (12.5–29 nmol/L) and mild (30–50 nmol/L) deficiency.1
Seasonal variability
At a population level, 25(OH)D levels can be described with a sinusoidal curve. There is substantial seasonal variability, with 25(OH)D levels at the end of summertime being around twenty–35 nmol/L higher than at the terminate of winter.3 There are as yet no data of which the authors are aware that relate the duration of deficiency, that is the proportion of time in a given year spent under a threshold of fifty nmol/L, and health outcomes. Nonetheless, it is critical to take into business relationship the time of year that a patient's 25(OH)D level is measured when interpreting vitamin D levels and making management choices. For example, a patient who is mildly vitamin D deficient at the stop of summer will most probable be deficient all year circular, and the deficiency will become more than severe during winter. Therefore vitamin D supplementation might exist needed. In contrast, for someone who is mildly deficient at the end of winter, a suggestion to slightly increase sun exposure at advisable times of the day might be sufficient.
Vitamin D and musculus part
Muscle weakness can be a sign of vitamin D deficiency.four The mechanism of this is unclear. It has been postulated that effects are mediated through actions of 1,25(OH)twoD on vitamin D-specific nuclear receptor in muscle tissue,5 but the presence of such receptors has recently been questioned.6 Regardless of mechanism, poor muscle function from vitamin D deficiency may affect further on musculoskeletal wellness by predisposing to college falls risk with resulting fracture (Meet afterward section). At that place is evidence in older adults that vitamin D affects factors straight related to muscle strength and function.5 This includes prospective information demonstrating that elderly men and women with baseline serum 25(OH)D levels <25 nmol/L, were ii.57 times more than likely to lose >40% of their grip strength and over 3% of their muscle mass over a iii year period.vii A contempo meta-analysis of 17 randomised controlled trials (RCTs) involving 5072 adults demonstrated improvements in muscle strength only with vitamin D supplementation in studies in which the mean baseline 25(OH)D level of participants was <25 nmol/50 (four studies, 465 participants),8 suggesting that most benefit is obtained in people with moderate to severe deficiency.
Vitamin D related osteomalacia
Osteomalacia is a bone disorder in adults in which osteoid, the newly formed bone matrix, does non mineralise. Clinical symptoms include bone hurting, muscular weakness (particularly proximal muscle weakness) and difficultly with walking.ix Fractures may occur due to bone fragility. Radiological changes besides include pseudofractures (Looser'south zone, Effigy 1), which appear as a radiolucent line through os cortex ofttimes with marginal sclerosis. Vitamin D deficiency is one cause of osteomalacia but vitamin D levels unremarkably need to be very depression (<25 nmol/50, oftentimes <12.5 nmol/L),nine to crusade clinical osteomalacia. Other causes of osteomalacia include very depression calcium intake and hyposphataemia from a range of causes. Furthermore, older adults consuming inadequate dietary calcium with low serum vitamin D levels tin develop both osteoporosis and osteomalacia,2 although the precise prevalence of osteomalacia in patients with hip fracture is unclear due to substantial differences in how osteomalacia is histologically divers in unlike studies.10
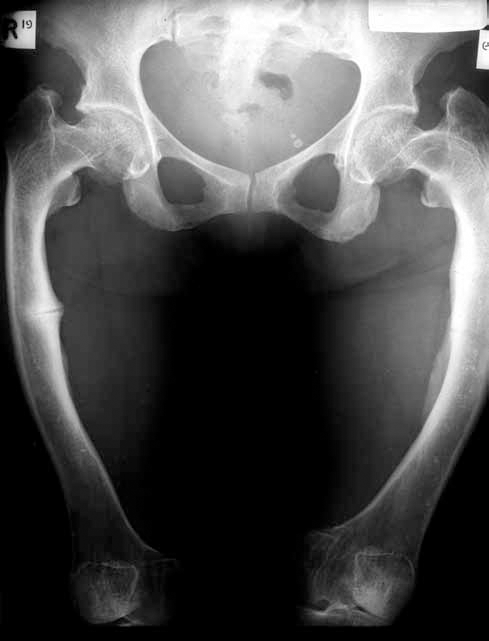
Figure 1. Looser's zone (pseudofracture) in osteomalacia. There is a radiolucent line through the medial right femoral cortex with some sclerosis at its margins
Osteoporosis, falls and fracture
Central letters
For maximal primary fracture prevention in the elderly, acceptable vitamin D levels and dietary calcium intake are both needed.
The benefits of supplementation are probable to exist greater in those with vitamin D deficiency and/or low dietary calcium intakes.
Low bone mineral density and falls are both hazard factors for osteoporotic fractures.11 Serum vitamin D has been shown to be associated with both these risk factors in observational studies. In cross-sectional studies, serum vitamin D in the range 30–90 nmol/Fifty has been positively correlated with hip bone mineral density in the elderly,12 but no clear threshold value has been established across which the relationship disappears. Most RCTs with bone density outcomes have given calcium and vitamin D concurrently, and overall effects on os mineral density take predominantly been modest and mostly occurred in the offset year of handling. Low serum vitamin D has also been associated with falls in observational studies.13,14 Chiefly, this association has been confirmed past RCT data. A meta-analysis of RCTs of vitamin D supplementation in the elderly (whether customs dwelling or in institutions) demonstrated a reduction in falls risk of nineteen% with doses of vitamin D of 700–1000 IU/day (pooled relative risk [RR] 0.81; 95% CI: 0.71–0.92 from seven studies, northward=1921) with no effects at lower doses (two studies, due north=505).15 In improver, a subgroup assay showed a 23% risk reduction (pooled RR 0.77; 95% CI: 0.65–0.ninety) if serum 25(OH)D levels above 60 nmol/L were achieved, only no reduction in adventure if achieved levels were <lx nmol/Fifty. Consistent with this, a meta-assay of studies performed just in community dwelling older people demonstrated a reduction in falls-take chances only in studies whose participants were selected on the basis of depression serum vitamin Dsixteen and a separate meta-assay of studies in older people in nursing care facilities or hospitals showed a reduction in rate of falls.17 Ane more contempo RCT has raised concerns regarding the safety of intermittent mega doses of vitamin D in the elderly, as such a regimen increased falls and fracture risk18 (Encounter adverse affects of vitamin D).
Given that vitamin D may exert furnishings through improved musculus role and falls hazard reduction and bone density effects, substantial weight in clinical decision making needs to exist given to studies with fracture outcomes as endpoints, and so equally to encompass the possible benefits or detriments of the total range of vitamin D effects. There is also potential for an interplay betwixt calcium intake and vitamin D with very low levels of calcium intake causing secondary hyperparathyroidism with increased 1,25(OH)2D which in turn may crusade increased breakdown of 25(OH)D.x
| Table 1. Specific molecules often included under the generic term 'vitamin D' | |
| Vitamin D3 (cholecalciferol) | Formed in skin from UV exposure and main grade found in vitamin D supplements |
| Vitamin D2 (ergocalciferol) | Produced by UV irradiation of the plant steroid ergosterol. Plant in some supplements |
| 25-hydroxyvitamin D [25(OH)D] | Produced in liver from vitamin D2 and Diii Serum level used to measure vitamin D status |
| 1,25 dihydroxyvitamin D [one,25-(OH)twoD] (calcitriol) | Biologically agile grade of vitamin D, produced past hydroxylation of 25(OH)D by kidneys |
Several systematic reviews accept addressed the interplay of calcium and vitamin D on fracture outcomes (Tabular array 2). Tang et alxix reviewed trials of calcium or calcium in combination with vitamin D. In 17 trials with over 52 000 participants, in trials giving calcium alone at that place was no statistically significant subtract in fracture take a chance but in trials of calcium and vitamin D given in combination there was a statistically pregnant 13% take chances reduction. Furthermore, in the subgroup of studies where vitamin D was co-administered, a dose in excess of 800 IU/solar day was needed to produce an outcome (take chances reduction of 16%). Greater effects were seen studies with a low hateful baseline serum vitamin D (Tabular array ane), although the p-value of 0.06 for the departure in effects was not statistically meaning. No difference in effect size was seen if a cut-off of fifty nmol/L was used. This suggests that benefits were more pronounced with more severe levels of vitamin D deficiency. Unsurprisingly, in studies in which compliance with treatment was loftier (>eighty%), the risk reduction was more marked at 24%.18 Other meta-analyses have compared the effects of vitamin D solitary compared to vitamin D given with calcium on fracture risk20–22 and consistently demonstrated that for there to exist a reduction in fracture risk, it is necessary that vitamin D and calcium are administered together and that vitamin D alone is insufficient to reduce fracture risk. Again, the potential for intermittent mega-dose vitamin D supplementation to result in increased falls and fracture should be noted.18
| Table two. Fracture hazard reduction from meta-analyses of RCTs of vitamin D alone and of vitamin D combined with calcium* | |
| All fractures | Relative risk |
| Tang, 200719 | |
| Calcium alone (due north=6517) | RR 0.90 (0.80–1.00)a |
| Calcium and vitamin D (n=46 108) | RR 0.87 (0.77–0.97) |
| Vitamin D <800 IU/twenty-four hours (northward=36 671) | RR 0.87 (0.71–i.05)b |
| Vitamin D ≥800 IU/day (n=9437) | RR 0.84 (0.75–0.94) |
| Serum 25(OH)D <25 nmol/L (n=ten 144) | RR 0.86 (0.78–0.93)c |
| Serum 25(OH)D ≥25 nmol/L (north=39 167) | RR 0.94 (0.90–0.99) |
| DIPART, 201020 (n=68517) | |
| Vitamin D lonely | Hr one.01 (0.92–1.12) |
| Vitamin D with calcium | Hour 0.92 (0.86–0.99) |
| Hip fracture | |
| Boonen, 200722 | |
| Vitamin D alone (n=9083) | RR i.10 (0.89–1.36)d |
| Vitamin D with calcium (n=45 509) | RR 0.82 (0.71–0.94) |
| Avenell, 200521 | |
| Vitamin D alone (n=18 668) | RR ane.17 (0.98–ane.41) |
| Vitamin D with calcium (n=ten 376) | RR 0.81 (0.68–0.96) |
| * Assuming denotes statistically meaning, 95% CI does not include 1.00; RR = relative risk; HR = gamble ratio a. No statistically pregnant difference in event between the two groups, but a statistically significant effect was only seen in with calcium and vitamin D combined b. p=0.03 for difference between <800 IU and ≥800 IU studies c. p=0.06 for divergence between <25 nmol/L and ≥25 nmol/50 groups d. Indirect comparison gives an RR reduction of 25% for vitamin D with calcium vs vitamin D lone (p=0.021) | |
The part of vitamin D and calcium in secondary fracture prevention
Key messages
Vitamin D and calcium supplementation alone are inadequate for secondary fracture prevention. But optimal vitamin D levels and acceptable calcium intake are needed to maximise effectiveness of anti-resorptive therapy for preventing further fractures.
The studies in the meta-analysis discussed were for master fracture prevention, ie. prevention of the start osteoporotic fracture, with the exception of the RECORD study.23 This 4-arm, secondary prevention trial compared vitamin D3 (800 IU/24-hour interval), one thousand mg calcium, vitamin D3 (800 IU/day) with calcium (1000 mg/day) and placebo in 5292 mobile people (85% female) aged >70 years who had already sustained a low-trauma fracture. The incidence of new, depression-trauma fractures did not differ significantly betwixt groups. Compliance with treatment was low in this report (<50% people took tablets on >80% of days), merely even in those participants with >80% compliance, no effects were seen.
RECORD demonstrates that calcium and vitamin D are insufficient by themselves for secondary fracture prevention. Withal, calcium and vitamin D still have an important role in secondary fracture prevention every bit an adjunct to specific anti-osteoporosis therapies. Well-nigh such therapies (eg. bisphosphonates) accept been evaluated in the context of adequate vitamin D levels and calcium intake. In a retrospective observational written report in 1515 postmenopausal on anti-resorptive therapies (alendronate, risedronate and raloxifene), the women who were vitamin D deficient (serum 25(OH)D ≤50 nmol/L) were more probable to sustain a fracture that those who were vitamin D replete (adapted odds ratio 1.77; 95% CI: 1.twenty–ii.59; p=0.004). Therefore optimal vitamin D levels seem necessary to maximise the anti-fracture efficacy of anti-resorptive agents.24 No studies have similarly investigated the impact of calcium repletion on fracture outcomes. However, calcium supplementation, in addition to vitamin D and alendronate in healthy postmenopausal women with depression BMD with a dietary calcium intake of ≥800 mg/day did non result in whatsoever added benefit for BMD,25 indicating that providing additional calcium to this population is not necessary. Significant questions have been raised virtually the prophylactic of calcium supplements due to possible increases in cardiovascular events.26 Therefore, for secondary prevention it is suggested that:
- serum 25(OH)D and dietary calcium intake are checked before initiating anti-osteoporosis therapy
- that calcium supplements are given if an adequate dietary calcium intake cannot be attained, and
- that vitamin D supplementation is essential if vitamin D levels are inadequate.11
Adverse effects of vitamin D: caution required with mega-dose therapy
Until recently, the agin effects of vitamin D were predominantly considered to be those of relatively astute toxicity with associated hypercalcaemia; namely nausea, vomiting, constipation, anorexia, apathy, headache, thirst, sweating and polyuria. At that place is as well a risk of renal and cardiovascular impairment through ectopic calcification, specially in the presence of hyperphosphataemia.27 Nevertheless, such effects are typically seen only at very high doses of vitamin D – suggested to be in excess of 25 000 IU/mean solar day with corresponding 25(OH)D levels of almost 500 nmol/L2 and are highly unlikely with normal therapeutic doses.
More than recently, other safe concerns accept emerged with less extreme levels of serum 25(OH)D/vitamin D doses. Notably, mega-dose intermittent oral vitamin D3 (500 000 IU once per year in fall) has been associated with a higher adventure of both falls (incidence RR 1.15; 1.02–i.xxx; p=0.03) and fractures (incidence RR 1.26; 95% CI: 1.00–i.59; p=0.047).eighteen This was reported in a double-bullheaded, placebo-controlled RCT of a single annual dose of 500 000 IU of vitamin D3 administered orally each autumn to winter for three–five years in 2256 community-dwelling older women aged 70 years or older and considered to be at high run a risk of fracture. For both falls and fracture, the greatest hazard was seen in the first iii months afterward dosing. This coincided with the substantial increment in serum vitamin D levels seen after each dose. Serum 25(OH)D was measured in a subsample of 137 participants. The median serum 25(OH)D rose from 49 nmol/L to approximately 120 nmol/L 1 month subsequently taking the vitamin D supplement and at iii months serum 25(OH)D remained high (approximately 90 nmol/Fifty). Moreover, a quadratic relationship was seen between changes in hip flexion force and the percent change in serum 25(OH)D. At vitamin D increases of less than 100%, hip forcefulness increased but with vitamin D increases above this level (equivalent to 120 nmol/L), hip flexion force decreased, providing a potential mechanism for the increased risk in falls and fractures.
In general, vitamin D3 supplements in RCTs (predominantly in elderly women in institutions and dependent intendance) are associated with lower mortality.28 However, of concern is the indication of a U-shaped relationship for serum vitamin D with bloodshed. A 50% higher full mortality rate has been observed in older men living in The Netherlands, in the lowest 10% of the distribution of plasma 25(OH)D (<46 nmol/Fifty) as well equally the highest 5% (>98 nmol/50) of the distribution.29
Preventing vitamin D deficiency: population advice
For most adults in Australia, dietary sources provide only a small (5–ten%) part of their vitamin D requirement. The primary source of vitamin D is exposure of the skin to sunlight (UV light). Advice to promote some lord's day exposure to allow the skin to manufacture vitamin Diii is of import to maintain acceptable serum 25(OH)D levels in the full general community. This communication may exist peculiarly of import to individuals with known depression levels of sun exposure who may demand to make a particular effort to achieve some exposure to sunlight (eg. indoor workers).
The minimal erythemal dose (MED) is the amount of UV exposure that just causes faint erythema. This varies with latitude, flavor, time of day, clothing and skin pigmentation. The current vitamin D and wellness in adults in Australia and New Zealand position statement1 provides a guide for sun exposure times (minutes) which result in one-third MED for people with moderately off-white pare at times of day that are useful for making vitamin D in different regions. If people expose around fifteen% of body surface (artillery and easily or legs) for this amount of time on most days, this should be equivalent to around yard IU/day of vitamin D3. However, chiefly, sun exposure communication has to be tempered with the demand to avoid excessive lord's day exposure associated with increased pare cancer take chances. Current Cancer Council recommendations are that most Australians need sun protection to prevent pare cancer when the UV alphabetize is 3 or above.30
Sun exposure guidelines for the general population
Suggested dominicus exposure guidelines for moderately blanched individuals who are not otherwise at increased run a risk of skin cancer are given in Table 3. In summer, vitamin D levels are likely to be exposing the easily, face up and arms for 6–7 minutes mid-morning or mid-afternoon on most days. In winter, advice is more circuitous, depending on latitude. In the far north of Australia, the UV alphabetize remains moderate to loftier throughout the year, remaining as high equally 7–8 in June in Darwin for example,31 and unprotected dominicus exposure around apex should be avoided year round. In winter in Brisbane, sun exposure at times further from noon may issue in a lower product of vitamin D. Yet, while the UV alphabetize around noon may be above 3,31 the gap betwixt the time needed to proceeds one- third MED (11 minutes) and the time for conspicuously chancy levels of sun exposure (ane MED) (34 minutes) is higher in winter.32 Therefore for most people, the short length of exposure required at apex for adequate vitamin D production (as given in Table 3) will be depression risk. In winter in southern Commonwealth of australia, sun exposure at midday for 15–29 minutes (depending on breadth) with as much blank skin exposed as feasible, on most days, is probable to exist helpful.one Exposing more skin in winter will increment vitamin D product.33
| Table 3. Dominicus exposure guidelines – Australia | |
| Season and location | Advice |
| Summer (all latitudes) | Easily, face and arms exposed for 6–7 minutes mid-morning or mid-afternoon on well-nigh days |
| Winter | |
| Northern Australia, eg. Darwin, Cairns, Townsville | Hands, face and artillery exposed for nine–13 minutes mid-morn or mid-afternoon on most days35 |
| Central Commonwealth of australia, eg. Brisbane, Perth | Hands, face and artillery exposed for 11 (Brisbane) to 15 (Perth) minutes around apex on most days |
| Southern Australia – Sydney to Hobart | Exposure of as much bare skin as viable around noon near days. Duration dependent on latitude – from sixteen (Sydney) to 29 minutes (Hobart) |
While 1 would expect broad spectrum sunscreens to reduce vitamin D production by blocking UV radiation, this may not bear witness to be the case in practice,34 perchance due to inadequate application. To maximise vitamin D product for the limited periods of sunday exposure given in Table 3, utilize of sunscreen may not be necessary, but otherwise advisable sun protective behaviours should be applied.
These guidelines may non guarantee sufficiency in everyone. For example, in Tasmania the prevalence of vitamin D deficiency (≤50 nmol/Fifty) was still 43% among the subgroup of healthy adults who were nearly sun seeking (reported sun exposure of >4 hours a 24-hour interval during weekends and holidays).3 As a event, specific recommendations for Tasmania were adult (See factsheets at www.cancertas.org.au/healthy-living/sunsmart) particularly drawing attention to times of yr where the UV index is moderate (late summer to early on autumn and early to mid spring) because vigilance during this period tin can reduce the winter dip in vitamin D levels, which is of particular importance in Tasmania.
Modifications of advice for at risk groups
Vitamin D deficiency is common in the elderly. The prevalence of deficiency defined as serum 25(OH)D <50 nmol/50 in a community habitation population-based sample of people over the age of 50 years in Tasmania was 45%.36 Some elderly populations are at college run a risk of vitamin D deficiency and potentially of poor bone health every bit a result of this deficiency. This includes elderly and/or disabled people in low and high level residential care;37 dark-skinned people,38 specially migrants or if pocket-sized wearing apparel is worn;38 people with a disability or chronic affliction, eg. multiple sclerosis;iii fair-skinned people and other people at risk of pare cancer who avert sun exposure.39 For instance, 86% of women and 68% of men in a sample of older people in residential anile intendance facilities in the northern Sydney area had a serum 25(OH)D level <28 nmol/L.forty Tailoring of dominicus exposure advice according to the specific requirements of these groups may exist necessary. In particular, for dark-skinned individuals the duration of dominicus exposure to attain adequate vitamin D levels is 3–6 times that described for fair-skinned people. In other loftier risk groups, eg. elderly in residential intendance,41 people with pare cancer or with weather condition resulting in photosensitivity, increases in sunday exposure may not be safe or feasible and supplements may exist needed.
Who to test?
Population screening for vitamin D deficiency in older adults by measuring serum 25(OH)D is not recommended, but testing loftier risk groups is appropriate. This includes people with known osteopenia and primary or secondary osteoporosis and the at risk groups described. If access to testing is a substantial barrier to seeking handling, it may be justified to treat adults who are at very loftier risk of vitamin D deficiency without testing to confirm deficiency. In this situation, it is suggested that the same dose used to treat moderate to severe deficiency is given.1
There is the potential for significant variability in exam results, especially between laboratories, and at the analytically important range (<50 nmol/L) of the assay. Clinicians should be aware of the imprecision of current 25(OH)D testing and exercise caution when interpreting results in clinical practice.
Correcting vitamin D deficiency
Mild vitamin D deficiency may exist corrected with increased sun exposure. However, where this is not possible or viable, or in the case of moderate to severe deficiency, correction is best achieved past the use of vitamin D supplements. One suggested regimen is 3000–5000 IU vitamin Diii daily for 6–12 weeks, checking levels after 12 weeks. Well-nigh people will need ongoing treatment at a maintenance dose of 1000–2000 IU/day. If this does non right deficiency, rule out underlying gastrointestinal disorders such as coeliac affliction.
Higher intermittent doses of vitamin D have been used and will correct deficiency. This may be useful where adherence to treatment is a major trouble. Even so, such preparations (containing 50 000 IU vitamin D3) are non routinely available in Commonwealth of australia and prescribing permission needs to be obtained from the Therapeutic Appurtenances Administration (come across www.tga.gov.au/hp/access-authorised- prescriber.htm#about) unless they are obtained from compounding chemists, although quality control is an outcome in this context. Rubber issues as described should also be considered before taking such an approach.
Every bit low calcium intakes and associated hyperparathyroidism increases the degradation of vitamin D compounds, a daily intake of 1000–1300 mg calcium per 24-hour interval, preferably using calcium-rich foods should besides be encouraged.
Disharmonize of interest: none declared.
References
Source: https://www.racgp.org.au/afp/2012/march/vitamin-d-and-the-musculoskeletal-health-of-older
0 Response to "what nutritional deficiency contributes to osteoporosis in older adult patients?"
Post a Comment